 
How is ankylosing spondylitis diagnosed?Įarly diagnosis is very important with ankylosing spondylitis. Patients are also prone to an onset of arthritis in the large joints and elsewhere, and can – in some cases – experience heel pain related to Achilles tendonitis, lung problems (as a result of lung scarring and spinal inflammation, limiting chest expansion), aortitis (inflammation of the aortic valve and the aorta – the large artery exiting from the left side of the heart), and uveitis, which can lead to visual loss. If left untreated, the ankylosing process can result in a "hunchback" appearance. Some patients experience similar pain in the buttocks, hips, chest wall, upper back, and neck. This pain is usually relieved by physical activity and improves by the end of the day. Symptoms of ankylosing spondylitis vary from patient to patient, but they most commonly begin with the onset of low back pain and stiffness that is especially noticeable in the morning hours and after long periods of rest. Heart and lung problems can also be associated with ankylosing spondylitis but are fortunately less common. 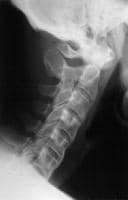
Uveitis (eye inflammation) can occur in this condition, and regular ophthalmology checkups are important, since eye damage can occur even before a person notices any symptoms. The second most common symptom is joint pain in the hips, shoulders, knees, chest wall, or other areas. The most common symptom of ankylosing spondylitis is low back pain and/or neck pain, morning stiffness and limited motion that is improved by exercise and unrelieved by periods of rest. What are the symptoms of ankylosing spondylitis? As noted above, having this genetic marker does not by itself mean a person has ankylosing spondylitis or any other inflammatory condition. People with the HLA-B27 genetic marker can develop other types of inflammatory conditions without developing AS, such as having eye inflammation with no accompanying arthritis. Many people with AS will not be able to identify anyone else in their family with the condition, however, since only about 20% of those with the HLA-B27 genetic marker will get an inflammatory condition such as AS. It is clear that some unidentified environmental trigger (and likely there is more than one type) plays a role in determining which people with this genetic marker end up developing ankylosing spondylitis.Ī number of people with AS will have a family history of the condition, although it may be much more painful and involve more areas of the body in one family member than another. 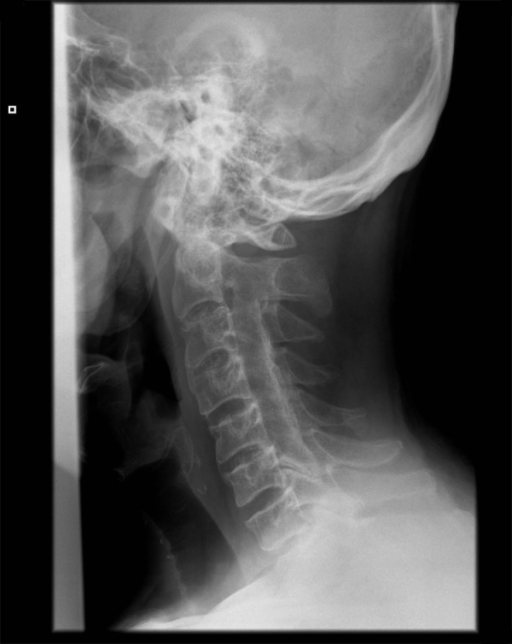
This marker does not appear to be the only cause, however, as 80% of people with this genetic marker never develop an inflammatory disease. More than 90% of people with ankylosing spondylitis have a particular genetic marker called HLA-B27, which can be found on their white blood cells. Genetics play a large role in this condition. AS can also affect children, called juvenile ankylosing spondylitis, and more commonly so in boys than girls. Side-view X-ray of an ankylosed spine Who gets ankylosing spondylitis?Īnkylosing spondylitis often begins at a young age (from the teens to the third decade of life) and is more common in men – about two to three times more common than in women. The neck (cervical spine) often has a similar inflammatory process and can likewise progressively lose motion. As a result of this inflammation, a person feels stiffness and pain in the back, a gradual loss of mobility, and in the most severe cases, a complete loss of motion of the lower back. "Spondylitis" refers specifically to the inflammatory process ("itis") of the spine. This leads to the fusion of one spinal vertebra to the one above or below it. In addition, inflammatory injury to bone tissue itself also causes scarring followed by bony overgrowth. This causes them to form scar tissue, and then new bone tissue can form within the ligaments. One component of this fusion process is that ligaments that connect one vertebra to another become injured by the inflammatory process. "Ankylosing" refers to the tendency of the spine to fuse (or “ankylose”). It can also cause inflammation at the entheses – areas where tendons attach to bone, such as where the Achilles’ tendon attaches to the heel or where the tendons at the elbow. The severity and pattern of joint involvement varies from person to person. But it can also affect several other joints, such as the hips, knees and chest wall. Ankylosing spondylitis (AS) is a chronic, inflammatory disorder that particularly affects the spine. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
